STARTING POINT: A HIDDEN PROBLEM
 Our main objective is to provide a clear and effective response to an endemic problem in the sector: the payment of all the medical interventions.
Our main objective is to provide a clear and effective response to an endemic problem in the sector: the payment of all the medical interventions.
After years of working together, we have found that the vast majority of doctors do not know the real situation of the state of their fees with insurance companies. Often, the bureaucratic machinery of the insurance companies, prevents medical centres from optimizing their collection of charges policy. In the worst cases, some of these medical assistances are never processed. AEHS, through our work program, we can clearly demonstrate to our clients, an improvement in their revenue and in their collection periods.
Due to the fact that each insurer has its own rules and conditions on the documentation to be submitted for invoice acceptance, accompanying demonstrative medical centre documentation is required.
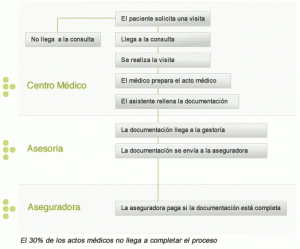
In this point, bureaucratic processes work in favour of the insurer, since a significant amount of medical assistance do not accompany the required documentation requested. The time frames offered by Insurance companies for the submission of demonstrative documentation (usually five days) are not usually sufficient for the average Medical Centre.
The conclusion is the core of the problem itself. The insurer only pays the invoices which come with the documentation 100% completed.

